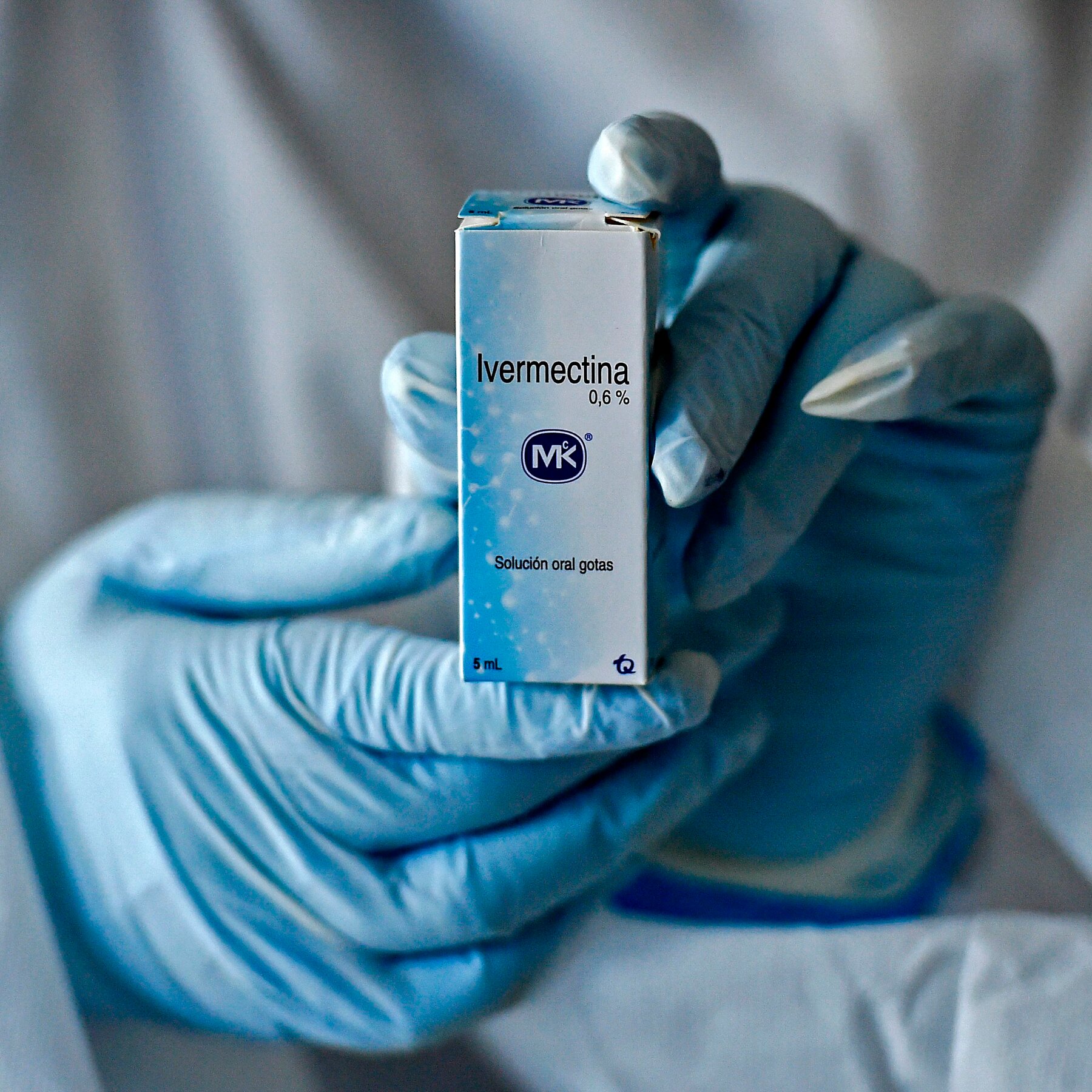
The COVID-19 pandemic, which began in late 2019, sparked an urgent global search for effective treatments. Amid the crisis, several existing medications were repurposed in hopes of curbing the disease’s progression. One such drug was ivermectin, a well-established antiparasitic used in both humans and animals for decades. Despite its proven efficacy against parasitic infections such as onchocerciasis, strongyloidiasis, and scabies, ivermectin’s off-label use in COVID-19 generated widespread controversy, debate, and misinformation.
The Rise of Ivermectin as a Potential COVID-19 Treatment
Ivermectin garnered global attention in 2020 after in vitro studies (lab-based experiments) suggested that it could inhibit the replication of SARS-CoV-2, the virus that causes COVID-19. These studies sparked interest due to ivermectin’s affordability, availability, and safety profile at approved doses.
Soon after, some clinicians, particularly in low- and middle-income countries, began prescribing ivermectin off-label for prevention and treatment of COVID-19. Proponents argued that it might reduce viral load, decrease inflammation, and prevent severe disease. Countries like India, Brazil, and parts of Africa incorporated ivermectin into treatment protocols at various stages of the pandemic, citing early observational data and anecdotal success.
Scientific Evaluation and Global Health Recommendations
Despite early enthusiasm, rigorous scientific evidence was lacking. Numerous studies conducted to evaluate ivermectin’s effectiveness for COVID-19 yielded mixed results. Some small-scale trials claimed benefits, but larger randomized controlled trials (RCTs)—the gold standard in medical research—often failed to replicate these findings.
Leading health organizations, including the World Health Organization (WHO), U.S. Food and Drug Administration (FDA), and the European Medicines Agency (EMA), reviewed the available evidence. Their conclusions were consistent:
Insufficient evidence to recommend ivermectin for COVID-19 prevention or treatment outside of clinical trials.
Warning against self-medication, especially with veterinary formulations, due to reports of toxicity, hospitalizations, and adverse effects.
In March 2021, the FDA issued a public advisory: “You are not a horse. You are not a cow. Seriously, y’all. Stop it,” referring to the misuse of veterinary ivermectin by humans, which became common in some areas.
The Misinformation Surge and Public Debate
The debate over ivermectin extended beyond science into the realm of politics, social media, and public trust. Advocates often cited conspiracy theories and accused regulatory agencies of suppressing ivermectin in favor of more expensive treatments or vaccines. On the other hand, critics highlighted the dangers of promoting unproven therapies without sufficient evidence.
Social media platforms became battlegrounds for the discussion, with viral misinformation campaigns spreading claims about ivermectin as a “miracle cure.” This led to hoarding, shortages for legitimate medical use, and public health risks due to inappropriate dosing and toxicity.
Conclusion
The off-label use of ivermectin during the COVID-19 pandemic was emblematic of the broader challenges faced during a global health emergency: fear, misinformation, politicization of science, and the desire for accessible treatments. While ivermectin remains a valuable antiparasitic drug, its role in COVID-19 treatment remains unproven by high-quality evidence. Moving forward, the global health community must continue to prioritize science, ethics, and clear communication to navigate future crises more effectively.